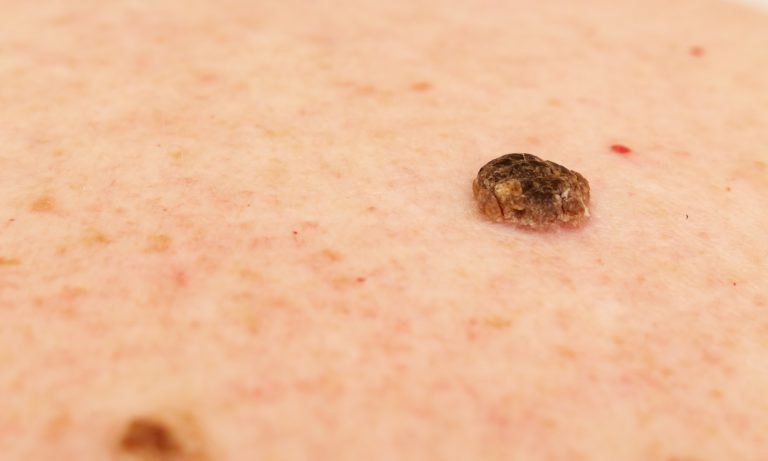
What is Neurofibromatosis?
Neurofibromatosis is a genetic disorder that affects the growth and development of nerve cells in the body. It is characterised by the formation of tumours on nerve tissue, leading to a variety of symptoms and complications. This condition can occur in different forms, with the two most common types being neurofibromatosis type 1 (NF1) and neurofibromatosis type 2 (NF2).
What are the types of neurofibromatosis?
There are three main types of neurofibromatosis, each with distinct characteristics and manifestations. Here are the types of neurofibromatosis:
- Neurofibromatosis Type 1 (NF1): Neurofibromatosis type 1, also known as NF1 or von Recklinghausen disease, is the most common form of neurofibromatosis. It is caused by mutations in the NF1 gene and is characterised by the growth of multiple noncancerous tumours called neurofibromas along the nerves. These tumours can develop on the skin, nerves, and other organs. NF1 is often associated with other features such as café-au-lait spots (pigmented skin patches), freckling in specific areas of the body, skeletal abnormalities, and optic nerve glioma (tumours of the optic nerve).
- Neurofibromatosis Type 2 (NF2): Neurofibromatosis type 2, abbreviated as NF2, is less common than NF1. It is caused by mutations in the NF2 gene and primarily affects the nervous system. NF2 is characterised by the development of bilateral vestibular schwannomas, which are tumours that grow on the nerves responsible for balance and hearing. Individuals with NF2 may experience hearing loss, tinnitus (ringing in the ears), balance problems, and facial weakness or numbness. In addition to vestibular schwannomas, NF2 can also lead to other nervous system tumours such as meningiomas and spinal cord tumours.
- Schwannomatosis: Schwannomatosis is a rarer form of neurofibromatosis. It is characterised by the development of multiple schwannomas, which are tumours that grow on the Schwann cells that surround nerves. Unlike NF1 and NF2, schwannomatosis typically does not involve vestibular schwannomas. Individuals with schwannomatosis may experience chronic pain, numbness, and muscle weakness, and sensory disturbances due to the presence of these tumours. Schwannomatosis can occur sporadically or be inherited in an autosomal dominant pattern.
Neurofibromatosis causes
Neurofibromatosis is primarily caused by genetic mutations that affect the production and function of proteins involved in nerve cell growth regulation. The specific genetic changes responsible for neurofibromatosis can occur spontaneously or be inherited from a parent with the condition.
In NF1, the mutations in the NF1 gene result in a decrease or loss of function of the protein neurofibromin. This protein normally helps regulate the growth of nerve cells. Without functional neurofibromin, there is increased growth of cells, leading to the formation of neurofibromas or bumps on the skin and other tissues.
In NF2, mutations in the NF2 gene cause a loss of function of the protein called Merlin or Schwannomin. This protein plays a role in suppressing cell growth. The absence of functional merlin protein leads to the uncontrolled growth of Schwann cells, resulting in the formation of tumours on nerves, including vestibular schwannomas.
Neurofibromatosis symptoms
The symptoms of neurofibromatosis can vary widely among individuals, even within the same family. Here are some common symptoms associated with neurofibromatosis:
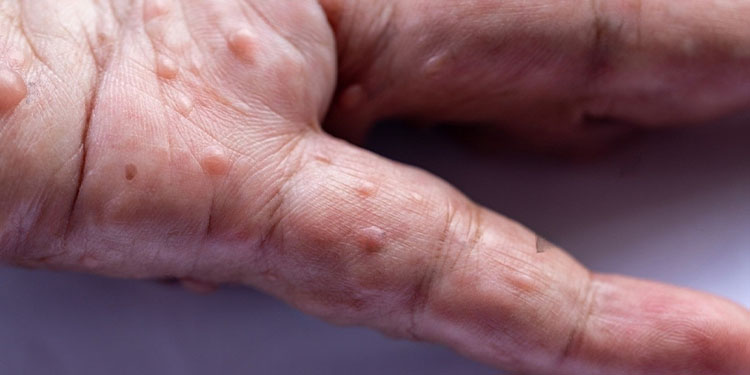
- Neurofibromas: One of the hallmark symptoms of neurofibromatosis is the development of neurofibromas. These are noncancerous tumours that grow on nerve tissue. Neurofibromas can appear as bumps or lumps under the skin, and their size and number can vary. They may cause cosmetic concerns or lead to discomfort if they press on nearby structures.
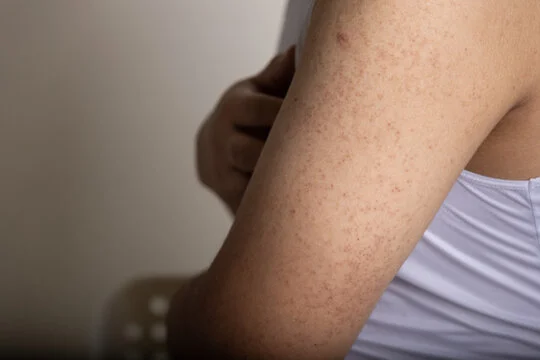
- Freckling: Freckling, particularly in the armpits or groin area, is another common symptom of NF1. These freckles may be darker than typical freckles and can be a characteristic feature of the condition.
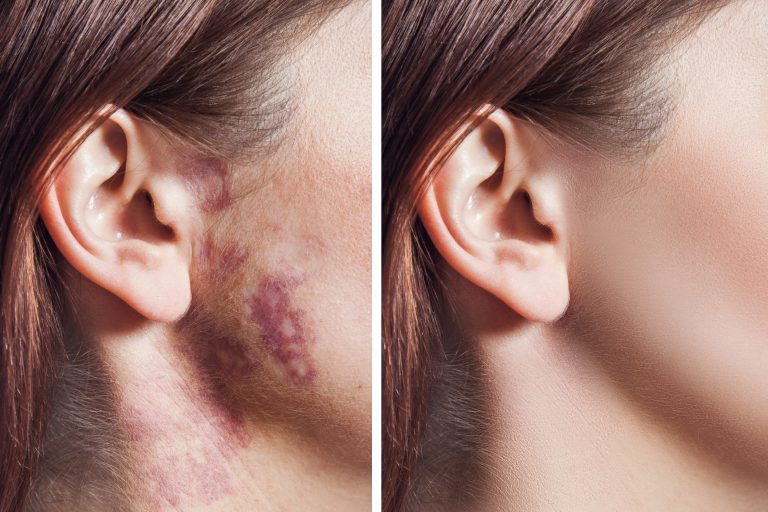
- Café-au-lait spots: Neurofibromatosis type 1 (NF1) is often characterised by the presence of café-au-lait spots. These are flat, pigmented skin patches that are usually light brown in colour. The size and number of café-au-lait spots can vary, and they may increase in number as a person gets older.
- Optic gliomas: In some cases of NF1, tumours can develop along the optic nerve, which carries visual information from the eyes to the brain. These tumours are known as optic gliomas and can lead to vision problems or other eye-related symptoms.
- Bone abnormalities: Neurofibromatosis can also affect the bones, leading to various skeletal abnormalities. These may include scoliosis (curvature of the spine), thinning or bowing of the long bones, and abnormalities in the shape or structure of certain bones.
- Hearing loss: Neurofibromatosis type 2 (NF2) is often associated with hearing loss. This occurs due to the growth of tumours on the nerves responsible for hearing, known as vestibular schwannomas or acoustic neuromas.
- Other nervous system involvement: Both NF1 and NF2 can involve the nervous system in different ways. This may include problems with balance, coordination, or muscle weakness.
How is neurofibromatosis diagnosed?
Diagnosing neurofibromatosis typically involves a combination of clinical evaluation, family history assessment, and genetic testing. Here is an overview of the diagnostic process for neurofibromatosis:
- Clinical Evaluation: A healthcare professional, often a geneticist or a neurologist, will conduct a thorough physical examination to look for characteristic signs and symptoms of neurofibromatosis. This includes assessing the presence of neurofibromas, café-au-lait spots, freckling, bone abnormalities, and other associated features.
- Family History Assessment: Gathering information about the presence of neurofibromatosis in the family is crucial for diagnosis. Neurofibromatosis can be inherited in an autosomal dominant pattern, which means that a person with the condition has a 50% chance of passing it on to each of their children.
- Genetic Testing: Genetic testing plays a key role in confirming the diagnosis of neurofibromatosis. It involves analysing a person’s DNA to identify specific genetic mutations associated with the condition. The two most common types of genetic tests used for neurofibromatosis are:
- NF1 Gene Testing: This test looks for mutations in the NF1 gene, which is associated with neurofibromatosis type 1 (NF1). It is the primary test used to diagnose NF1 and can identify mutations in approximately 95% of individuals with NF1.
- NF2 Gene Testing: This test examines the NF2 gene for mutations linked to neurofibromatosis type 2 (NF2). It is used to confirm the diagnosis of NF2 in individuals suspected to have this specific type of neurofibromatosis.
How is neurofibromatosis treated?
Since neurofibromatosis is a lifelong condition, a multidisciplinary approach involving various healthcare specialists is often recommended. The treatment options for neurofibromatosis may include:
- Surgery: Surgical intervention may be required in certain cases of neurofibromatosis. The type of surgery depends on the specific symptoms and complications. For example, surgery may be performed to remove neurofibromas that cause pain, disfigurement, or compress vital structures. In neurofibromatosis type 2 (NF2), surgical removal of vestibular schwannomas (acoustic neuromas) may be considered to preserve hearing and relieve associated symptoms.
- Medications: Medications may be prescribed to manage specific symptoms of neurofibromatosis. For example, pain medications can help alleviate discomfort caused by neurofibromas. Medications such as bevacizumab may be considered for certain cases of NF2 to reduce the size of vestibular schwannomas and improve hearing.
- Physical Therapy: Physical therapy and rehabilitation may be beneficial to address motor difficulties, muscle weakness, or balance problems associated with neurofibromatosis. These interventions aim to improve mobility, strength, coordination, and overall functional abilities.
- Optic Glioma Management: In cases where optic gliomas cause visual impairment or other complications, specialised treatments such as chemotherapy, radiation therapy, or surgery may be considered. The specific approach depends on the severity and location of the optic glioma.
- Genetic Counselling: Genetic counselling is recommended for individuals with neurofibromatosis and their families. Genetic counsellors provide information about the inheritance pattern, recurrence risks, and the availability of genetic testing.
Conclusion
If you suspect that you or a loved one may have a skin condition like neurofibromatosis, it’s crucial to seek professional medical advice. A dermatologist is a specialised doctor who can accurately diagnose and provide personalised treatment options for various skin conditions, including neurofibromatosis. Whether it’s managing symptoms, exploring surgical options such as plastic surgery, or seeking advice on how to get glowing skin, a dermatologist is the go-to expert.
If you’re looking for a local dermatologist in your area, we recommend visiting the Find Local Dermatologist webpage on the Skin and Hair Academy website, you can easily access a comprehensive directory of dermatologists near you.
Remember, early detection and proper medical care are essential in managing and treating skin conditions effectively. Don’t hesitate to take the next step and schedule a consultation with a dermatologist who can provide the expertise and guidance you need for optimal skin health.
FAQs on Neurofibromatosis
1) Why is Neurofibromatosis so painful?
Neurofibromatosis can cause pain due to neurofibromas, tumours that grow on nerve tissue. The size and location of these tumours can compress or irritate nerves, leading to varying levels of pain. Factors such as the number and size of neurofibromas and their impact on surrounding structures contribute to the severity of pain.
2) Is neurofibromatosis common?
Neurofibromatosis is relatively uncommon but not rare. It affects an estimated 1 in every 3,000 to 4,000 people worldwide. Neurofibromatosis type 1 (NF1) is more common than neurofibromatosis type 2 (NF2), with NF1 occurring in approximately 1 in 3,000 individuals, while NF2 occurs in about 1 in 25,000 to 1 in 40,000 individuals.
3) Can neurofibromatosis be removed?
Neurofibromas, the tumours associated with neurofibromatosis, can be surgically removed based on factors like size, location, and number of neurofibromas, as well as associated risks. Surgery may help alleviate pain, address functional impairments, or manage cosmetic concerns.
4) How do neurofibromas start?
Neurofibromas in neurofibromatosis develop from specific types of cells called Schwann cells, which are responsible for supporting and insulating nerves. Genetic mutations in genes associated with neurofibromatosis (such as the NF1 gene for NF1 or the NF2 gene for NF2) can disrupt the regulation of Schwann cell growth, leading to the formation of neurofibromas.
5) Can you live a normal life with neurofibromatosis?
Individuals with neurofibromatosis can lead fulfilling lives, despite the varying impact of the condition. With proper management, including regular medical care and appropriate treatments, they can pursue education, careers, relationships, and activities.