1. Causes of psoriasis
Psoriasis is considered to be an auto-immune disease, which primarily starts with a malfunction of the patient’s immune system. T cells, which are white blood cells, protect the body from diseases and infections. In psoriasis, these cells are activated by mistake, and start setting off other immune responses. Due to this, skin cells swell and start multiplying faster than normal. Psoriasis patients may sometimes notice their condition getting better for no evident reason, and also worsening on some other day without any explanation. Certain infections, drugs, weather changes and increased stress can trigger a psoriasis attack and can lead to a worsening of the condition.
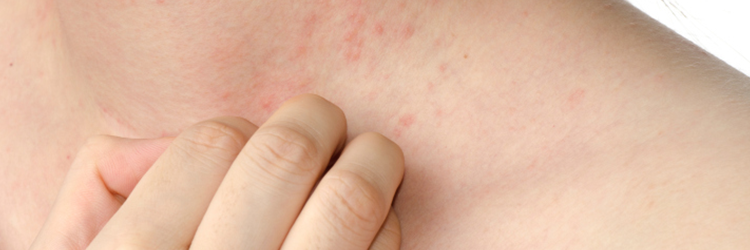
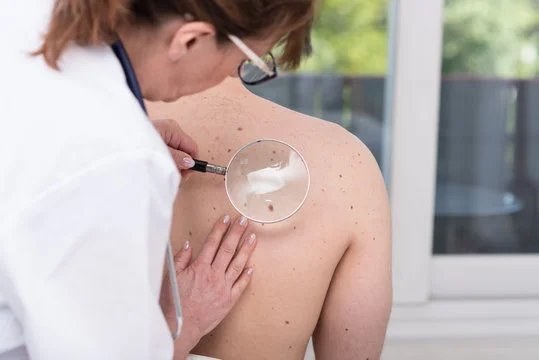
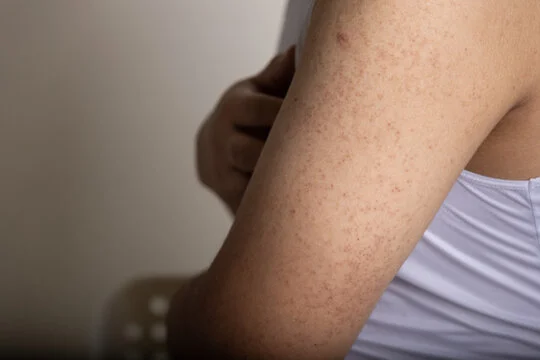
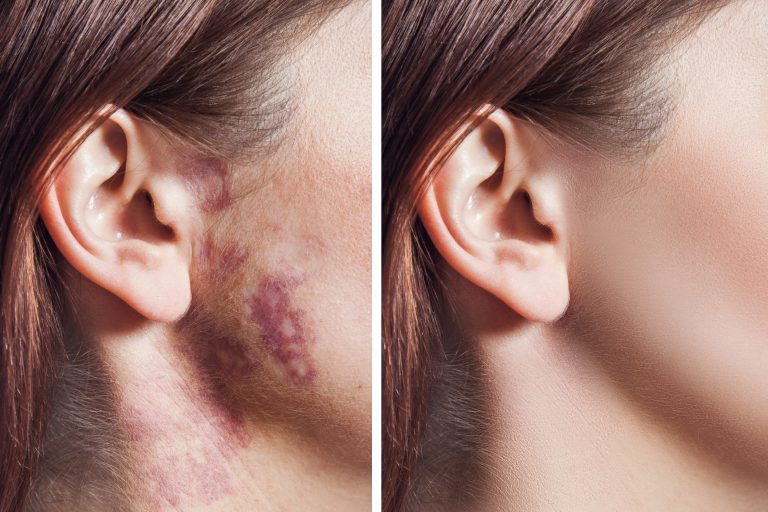
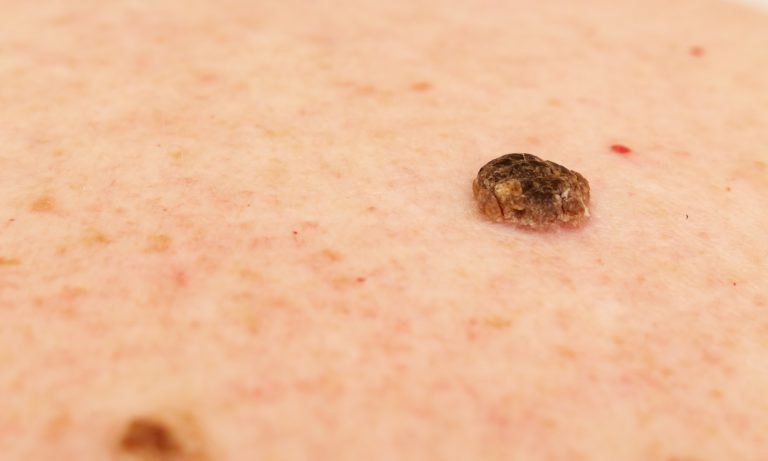
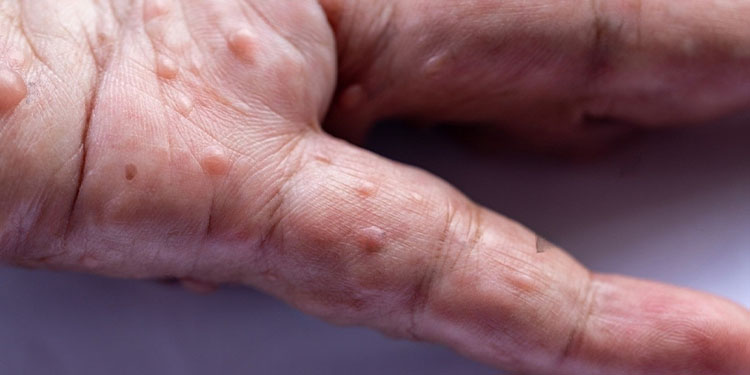
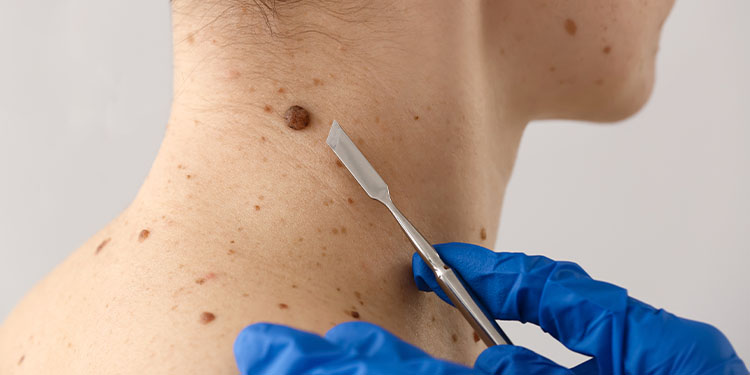
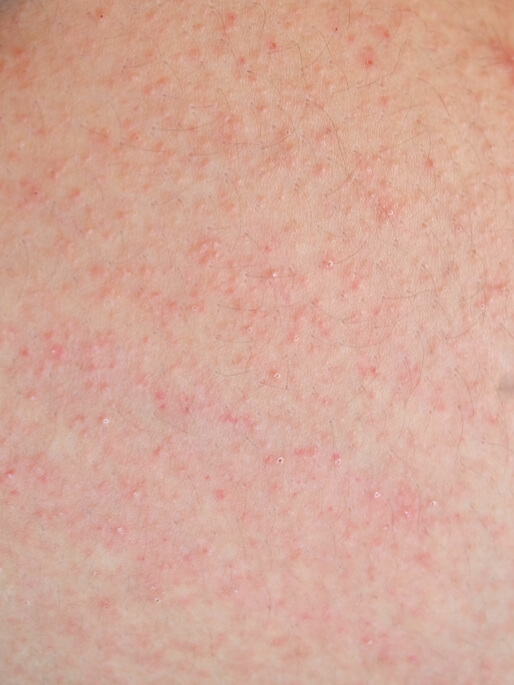
2. Symptoms of psoriasis
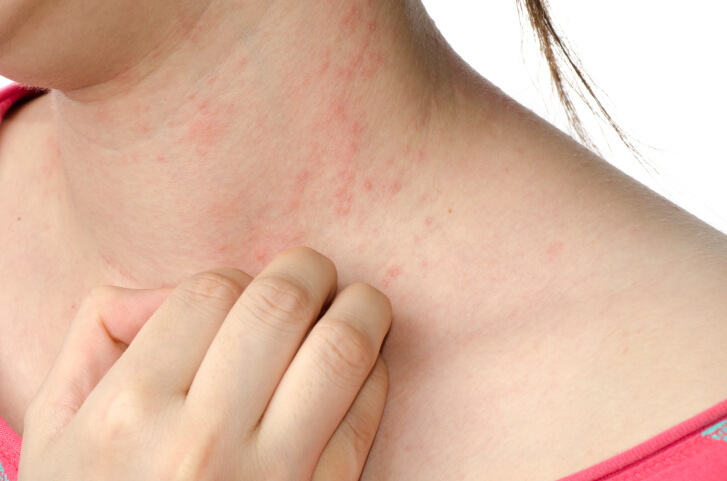
3. Caring for the skin of psoriasis patients
The best way to take care of the skin in psoriasis is to keep it moist with lotions, creams, baths and soaks. For mild psoriasis, OTC drugs containing aloe can be highly soothing. Avoid anything that triggers flare-ups, such as a skin injury, stress, anxiety, infection, over-exposure to sunlight, alcohol, smoking, and certain medicines like NSAIDs, and beta-blockers, among others. Over time, the patient will be able to identify the triggers, and avoid them altogether.
4. Cure for psoriasis
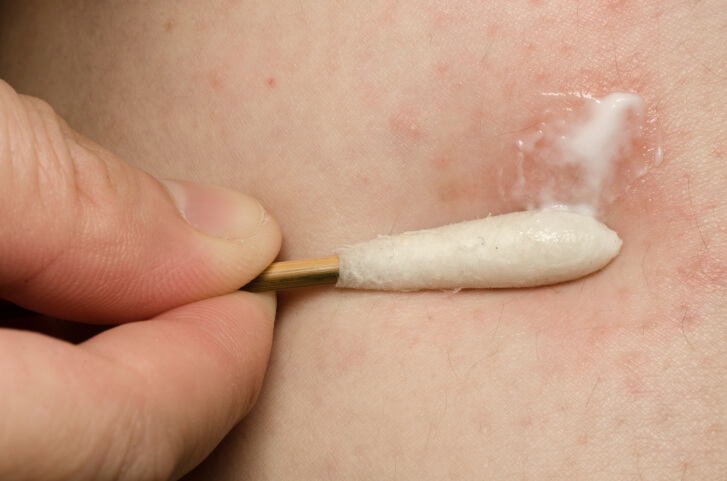
- Topical cure: There are certain creams and ointments that may be applied on the skin directly to soothe the condition.
- Emollients: Moisturizing treatment to reduce itching and scaling
- Steroid creams: Applied to cure mild to moderate psoriasis
- Vitamin D analogues: Calcipotriol, calcitriol and tacalcitol
- Dithranol: It helps suppress the production of skin cells.
- Calcineurin inhibitors including pimecrolimus and tacrolimus
- Light therapy: Artificial and natural UV light is sometimes used in for the treatment of psoriasis. PUVA is a combination of drugs that increases skin sensitivity to light and UV-A light, thus keeping the condition under control.
- Systemic treatment: In severe cases, shots may be given to the patient as part of the treatment regime.
Research is still being conducted to understand psoriasis in greater detail, and to chart out more effective treatment procedures. Currently, psoriasis treatment can continue throughout the patient’s life. Psoriasis patients must exercise a lot of caution in order to be able to lead a comfortable life.