Skin cancer is a prevalent condition that affects millions of people worldwide, with melanoma being one of its most aggressive and dangerous forms. Recognizing the symptoms, understanding the causes, and being aware of the available treatment options are crucial in combating this disease effectively.
In this article, we will delve into the intricacies of melanoma, answering the common question: “What is melanoma?” We will provide you with valuable insights to help you identify its symptoms, comprehend its underlying causes, and explore the various stages and treatment approaches. By the end of this article, you will possess the knowledge necessary to prioritize your skin health and take proactive measures in dealing with melanoma.
What is Melanoma Cancer?
Melanoma cancer is a highly aggressive and dangerous form of skin cancer that emerges from the melanocytes, the cells responsible for producing melanin, the pigment that gives color to our skin, hair, and eyes. When these melanocytes undergo malignant changes, they give rise to cancerous tumors known as melanoma.
What sets melanoma apart from other types of skin cancer is its potential to rapidly spread to other parts of the body, including vital organs, if left untreated. This aggressive nature makes it a serious and life-threatening condition that requires immediate attention.
Melanoma often originates in the skin but can also occur in other areas where melanocytes are present, such as the eyes, mucous membranes, or even internal organs. The primary cause of melanoma is excessive exposure to ultraviolet (UV) radiation, whether from the sun or artificial sources like tanning beds. Intense and intermittent exposure, especially leading to sunburns, poses a higher risk of developing melanoma.
It’s crucial to remember that melanoma can also appear in body parts that aren’t generally exposed to sunlight. This implies that additional factors, such as genetic predisposition and certain environmental stimuli, could affect how it develops. A person’s risk is increased if they have fair skin, a family history of melanoma, many atypical moles, or a compromised immune system.
Symptoms of Melanoma
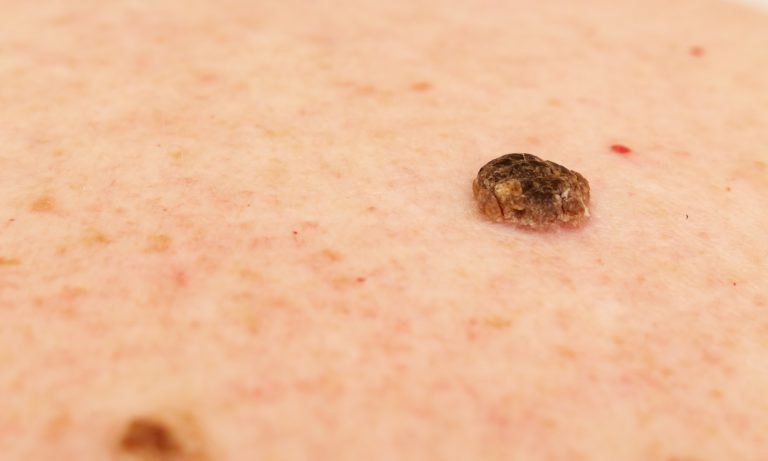
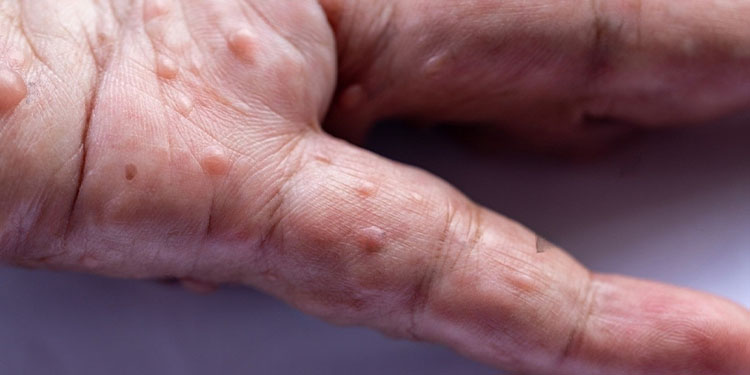
Melanoma can appear in various ways, and it is important to be vigilant and recognize any changes in your skin. Common symptoms of melanoma include:
- Asymmetrical moles: Melanoma lesions often have an irregular shape, with one half differing from the other half.
- Irregular borders: The borders of melanoma lesions may appear ragged, notched, or blurred.
- Changes in color: Melanoma lesions may exhibit various colors or have uneven shades of brown, black, red, white, or blue.
- Diameter: Melanoma lesions typically exceed the size of regular moles, with a diameter larger than 6 millimeters.
- Evolving appearance: Melanoma lesions can change in size, shape, or color over time.
- Itching, bleeding, or crusting: Melanoma lesions may cause itching sensations, bleed, or develop crusts, which could indicate potential malignancy.
Causes of Melanoma
Here are a few of the common causes of Melanoma:
- Excessive UV Radiation: Overexposure to ultraviolet (UV) radiation, whether from the sun or tanning beds, is a significant risk factor for developing melanoma. Intense and intermittent sun exposure, particularly leading to sunburns, poses a higher risk.
- Sun Exposure: While excessive UV radiation is a primary cause, melanoma can also occur in areas of the skin not regularly exposed to the sun. This suggests that factors other than direct sunlight exposure may contribute to its development.
- Family History: Having a family history of melanoma increases the risk of developing the disease. Genetic factors can play a role in predisposing individuals to melanoma.
- Atypical Moles: The presence of numerous atypical moles, also known as dysplastic nevi, is considered a risk factor for melanoma. These moles often exhibit unusual features, such as irregular borders, uneven coloration, or larger size.
- Fair Skin: Individuals with fair skin that burns easily are at a higher risk of melanoma. Fair skin has less melanin, a pigment that provides some protection against UV radiation.
- Weakened Immune System: A weakened immune system can compromise the body’s ability to defend against cancerous cells, including melanoma. Conditions such as HIV/AIDS, organ transplantation, or certain medications that suppress the immune system can increase the risk of developing melanoma.
- Previous Skin Cancer or Melanoma: A history of previous melanoma or other types of skin cancer increases the risk of developing subsequent melanomas. It is crucial for individuals with a history of skin cancer to be vigilant about regular skin checks and take precautions to minimize further risk.
Stages of Melanoma
Melanoma is staged based on the extent of the cancer’s spread, which helps determine the appropriate treatment approach. The stages of melanoma are typically categorized as follows:
- Stage 0 (Melanoma in situ): The melanoma is only in the top layer of skin (the epidermis). It has not invaded deeper layers or spread to nearby lymph nodes or distant sites.
- Stage I: This stage is characterized by a low-risk primary melanoma with no evidence of spread. The tumor is localized to the skin and has not spread to lymph nodes or distant sites.
- Stage II: In stage II, features are present that indicate a higher risk of recurrence, but there is no evidence of spread to lymph nodes or distant sites.
- Stage III: At this stage, the melanoma has spread to nearby lymph nodes or nearby skin, but it has not yet metastasized to distant sites.
- Stage IV: In this advanced stage, the melanoma has spread to more distant lymph nodes or skin, or it has metastasized to internal organs such as the liver, lungs, brain, bones, or other distant sites.
Diagnosis of Melanoma
The diagnosis of melanoma typically involves the following steps:
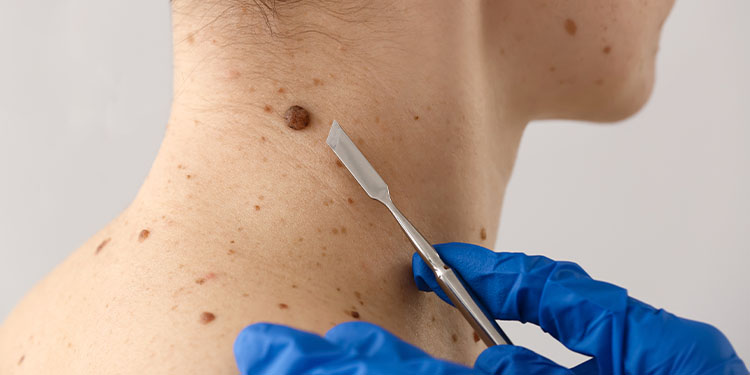
- Skin Examination: A thorough visual inspection of the skin to identify suspicious moles or changes.
- Dermatoscopy: Close examination of skin lesions using a dermatoscope to detect abnormal features.
- Biopsy: Removal of a sample of suspicious skin tissue for laboratory analysis.
- Pathology Analysis: Examination of the biopsy sample under a microscope to confirm melanoma and determine its characteristics.
- Staging and Imaging: Additional tests, such as imaging scans, to determine the extent of cancer spread.
Treatment Options For Melanoma
The following are common treatment options for melanoma, based on the provided references:
- Surgery: Surgery is the primary treatment for melanoma and involves removing the tumor and surrounding healthy tissue. Surgical options may include excision, lymph node biopsy or dissection, and reconstructive surgery.
- Immunotherapy: Immunotherapy stimulates the body’s immune system to recognize and destroy cancer cells. It includes drugs like immune checkpoint inhibitors (such as pembrolizumab and nivolumab) and cytokines (such as interleukin-2 and interferon-alpha).
- Targeted Therapy: Targeted therapy drugs are designed to attack specific genetic mutations or molecular features of melanoma cells. These medications may be prescribed for advanced or metastatic melanoma cases.
- Radiation Therapy: Radiation therapy uses high-energy X-rays or other forms of radiation to kill cancer cells or shrink tumors. It can be used as a primary treatment for localized melanoma or as adjuvant therapy after surgery to target remaining cancer cells.
- Chemotherapy: Although less commonly used for melanoma, chemotherapy drugs may be prescribed in certain cases, especially when melanoma has spread to distant organs. Chemotherapy uses drugs to kill cancer cells throughout the body.
Conclusion
To conclude, melanoma is a serious type of skin cancer. It can occur anywhere on the skin, including areas not regularly exposed to the sun. Detecting melanoma early is crucial for successful treatment, as it can spread to other parts of the body if left untreated. Regular skin examinations, self-checks, and prompt medical attention for any suspicious changes in moles or skin are essential for early detection and improved outcomes. If you have any concerns about your skin health, it is important to consult with a healthcare professional.
If you’re interested in learning more about skin diseases, skin inflammation, and related topics, Skin and Hair Academy is a valuable resource. Our website offers a wealth of informative blogs and articles that cover various dermatological conditions and their treatments. Additionally, Skin and Hair Academy provides a helpful feature to find the best dermatologists in your area. By visiting our “Find Local Dermatologist” webpage, you can easily locate a trusted dermatologist within your proximity for personalized care and expert advice.
FAQs
1) What is Melanoma caused by?
Melanoma is primarily caused by excessive exposure to ultraviolet (UV) radiation, both from sunlight and artificial sources like tanning beds. Intense and intermittent exposure, leading to sunburns, poses a higher risk of developing melanoma. Other factors, such as genetic predisposition and environmental influences, may also contribute to its development.
2) Is Melanoma cancer serious?
Yes, melanoma is a serious form of skin cancer. It has a higher potential to spread to other parts of the body compared to other types of skin cancer. Early detection and prompt treatment are crucial in improving outcomes and increasing the chances of successful recovery.
3) Is Melanoma curable?
Melanoma can be curable, especially when detected early and treated promptly. The prognosis and chances of cure depend on various factors, including the stage of the cancer, the thickness of the tumor, and whether it has spread to other parts of the body. Early detection plays a vital role in improving the chances of successful treatment.
4) Can Melanoma lead to death?
If left untreated or diagnosed at an advanced stage, melanoma can be life-threatening. It has the potential to metastasize (spread) to other organs, which can significantly impact a person’s prognosis. However, with early detection and appropriate treatment, the chances of survival and successful management of melanoma are significantly increased.
5) Can I live a normal life with Melanoma?
With proper treatment and regular follow-up care, many individuals with melanoma can live a normal life. However, it is essential to prioritize ongoing skin health and take necessary precautions to reduce the risk of recurrence or the development of new melanomas. This may involve regular skin examinations, sun protection measures, and ongoing surveillance by a dermatologist. Following a healthy lifestyle and seeking support from healthcare professionals can also contribute to maintaining a good quality of life while living with melanoma.