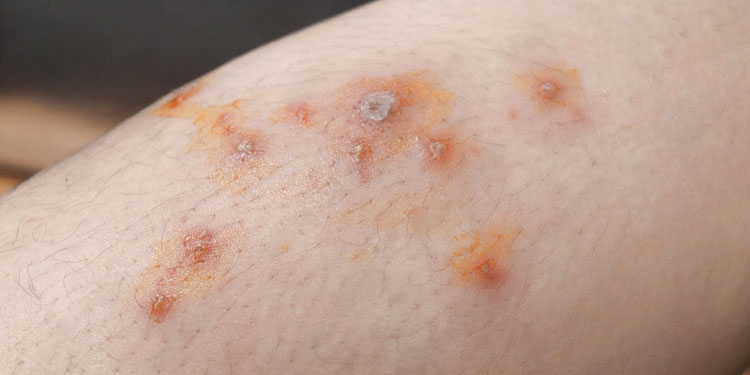
What is Impetigo?
Impetigo meaning can be described as a highly bacterial skin infection that primarily affects children but can also occur in adults. The bacteria that cause impetigo can enter the body through cuts, scrapes, insect bites, and openings in the skin, such as those caused by eczema, dermatitis, or other skin conditions. Impetigo is highly contagious and can spread quickly through direct contact with the sores or crusts. It can also be transmitted indirectly through sharing contaminated objects like towels, clothing, or bedding.
Types of Impetigo
Impetigo, a contagious bacterial skin infection, presents in various forms, including:
- Non-bullous Impetigo: This is the most common type of impetigo. It typically begins as small red sores or blisters that quickly burst, leaving behind a characteristic honey-coloured crust. These sores often appear around the nose and mouth, but they can also occur on other parts of the body. Non-bullous impetigo may be itchy and can spread through scratching, potentially leading to additional areas of infection.
- Bullous Impetigo: Bullous impetigo is less common and primarily affects infants and young children. It is characterised by larger, fluid-filled blisters that initially appear clear but eventually become cloudy or yellow. These blisters may be surrounded by red, itchy skin. Bullous impetigo can develop on various body sites and, similar to non-bullous impetigo, scratching can contribute to the spread of the infection.
- Ecthyma: Ecthyma is a more severe form of impetigo that extends deeper into the skin layers. It typically arises from untreated or inadequately treated non-bullous or bullous impetigo. Ecthyma presents as painful, fluid-filled blisters covered by thick, grey or yellowish crusts. In some cases, the crusts can lead to the formation of ulcers or shallow sores. Ecthyma commonly occurs on the lower legs, feet, or buttocks and may result in scarring after healing.
Impetigo is closely associated with other skin diseases and conditions. Scratching the blisters or crusts can increase the risk of developing cellulitis, a skin bacterial infection that affects the deeper layers of the skin.
Impetigo Symptoms
Impetigo presents with several distinct symptoms, which can vary depending on the type and severity of the infection.
- Red Sores or Blisters: Impetigo typically starts with the appearance of small red sores or blisters on the skin. These lesions may be itchy and can occur on various parts of the body, but they commonly develop around the nose and mouth. The blisters may be filled with fluid, which can later ooze and form a yellowish crust.
- Honey-Coloured Crusts: As the blisters burst, they leave behind a characteristic honey-coloured crust on the skin. The crusts may be slightly raised, dry, and easily detachable. Scratching the affected areas can contribute to the formation of more crusts and potentially spread the infection.
- Itching and Discomfort: Impetigo can cause itching and discomfort in the affected areas. The itching may intensify when the blisters or crusts are present, leading to a desire to scratch the skin. However, scratching should be avoided to prevent further complications or the spread of infection.
- Swollen Lymph Nodes: In some cases, impetigo may lead to swollen lymph nodes in the nearby area. Lymph nodes are small, bean-shaped glands responsible for filtering and trapping harmful substances or bacteria in the body. Swelling of these lymph nodes can be a sign of an immune response to the infection.
Impetigo can occur on healthy skin, but individuals with pre-existing skin conditions like dermatitis may be more susceptible to developing the infection.
Causes of Impetigo
Impetigo is primarily caused by bacteria that invade the skin and lead to infection. These bacteria can enter the body through various means and cause the characteristic skin lesions associated with impetigo
The primary causes and risk factors of impetigo include:
- Skin Breaks or Injuries: Impetigo bacteria can enter the body through cuts, scrapes, insect bites, or other skin injuries. When the skin barrier is compromised, it becomes easier for the bacteria to penetrate and cause infection.
- Skin-to-Skin Contact: Impetigo is highly contagious and can spread through direct contact with an infected individual. Touching, hugging, or sharing personal items like towels, clothing, or bedding with an infected person can transfer the bacteria to your skin and potentially cause impetigo.
- Pre-existing Skin Conditions: Individuals with pre-existing skin conditions, such as dermatitis, eczema, or other skin lesions, have a higher risk of developing impetigo. These conditions often cause inflammation, dryness, or breaks in the skin, providing an entry point for impetigo-causing bacteria.
- Poor Hygiene: Inadequate personal hygiene practices can contribute to the development and spread of impetigo. Failing to regularly wash hands, not properly cleaning and covering skin injuries, or using contaminated items can increase the risk of bacterial infection.
- Crowded Environments: Impetigo is more common in crowded environments where close contact among individuals is frequent. Schools, daycares, and sports teams are examples of settings where impetigo can spread easily from person to person.
Prevention of Impetigo
Here are some preventive measures you can take:
- Good Hygiene Practices: Regularly washing your hands with soap and water is one of the most effective ways to prevent impetigo. Make sure to wash your hands before eating, after using the restroom, and after coming into contact with someone who has impetigo.
- Keep Wounds Clean and Covered: Properly clean and cover any cuts, scrapes, or skin injuries to prevent bacteria from entering and causing impetigo. Use clean water and mild soap to cleanse the wound, apply an antibiotic ointment, and cover it with a sterile bandage.
- Avoid Sharing Personal Items: Refrain from sharing personal items such as towels, clothing, razors, and other items that may come into contact with your skin. Sharing these items can potentially spread impetigo-causing bacteria.
- Prompt Treatment of Skin Conditions: If you have a pre-existing skin condition, such as dermatitis or eczema, it is essential to manage and treat it promptly. Keeping your skin healthy and intact reduces the risk of impetigo development.
- Maintain Clean Environments: Regularly clean and disinfect surfaces and objects that may come into contact with the skin, especially in shared spaces like gyms, schools, and daycare centres. Pay attention to commonly touched surfaces like doorknobs, light switches, and exercise equipment.
- Promptly Seek Medical Attention: If you or your child develop symptoms of impetigo, such as red sores, blisters, or honey-coloured crusts, seek medical attention promptly. Early diagnosis and treatment can help prevent the spread of impetigo to others and reduce complications.
Impetigo Treatment
Treatment for impetigo typically involves a combination of self-care measures and medical interventions. The specific treatment approach may vary depending on the severity and type of impetigo. Here are common treatment options:
- Antibiotic Creams or Ointments: Topical antibiotics, such as mupirocin or retapamulin, are often prescribed for mild cases of impetigo. These medications should be applied directly to the affected areas as instructed by a healthcare professional.
- Oral Antibiotics: For more extensive or severe cases of impetigo, oral antibiotics may be prescribed. Commonly used antibiotics include dicloxacillin, cephalexin, or erythromycin. It is important to take the full course of antibiotics as prescribed by your healthcare provider to ensure complete eradication of the bacteria.
- Self-care Measures: Alongside medication, self-care measures can help manage and prevent the spread of impetigo. Gently cleanse the affected areas with mild soap and water, remove crusts using a clean cloth soaked in warm water, and keep the skin clean and dry.
- Preventing the Spread: To prevent the spread of impetigo, avoid scratching the affected areas and keep them covered with a sterile bandage. Wash your hands thoroughly after touching or treating impetigo sores. Avoid close contact with others until the infection is no longer contagious.
Conclusion
If you suspect or have been diagnosed with impetigo and require specialised care, it is advisable to consult with a dermatologist. Dermatologists are medical professionals with expertise in diagnosing and treating various skin conditions, including impetigo. They can provide personalised guidance and recommend the most appropriate treatment options for your specific case.
To find a local dermatologist near you, we recommend visiting the Find Local Dermatologist webpage on our website. The platform offers a comprehensive directory of qualified dermatologists in your area. By accessing this resource, you can easily locate a dermatologist who can assess your condition, provide professional advice, and guide you through the treatment process.
FAQs on Impetigo
1) What are the 3 types of impetigo?
The three types of impetigo are:
- Non-bullous impetigo: This is the most common type, characterised by small red sores or blisters that develop a honey-coloured crust.
- Bullous impetigo: Less common, it causes larger fluid-filled blisters that eventually form a yellowish crust.
- Ecthyma: A more severe form that penetrates deeper into the skin, causing painful blisters that develop into ulcers or sores covered by crusts.
2) Is impetigo serious?
While impetigo is generally not considered a serious condition, it can cause discomfort and inconvenience. However, if left untreated, it can lead to complications such as cellulitis (skin infection), deeper skin infections, or the spread of bacteria to other areas or individuals. Prompt treatment is important to prevent these complications.
3) How long does impetigo last?
With appropriate treatment, impetigo can start improving within a few days. Non-bullous impetigo usually heals within 1 to 2 weeks, while bullous impetigo may take slightly longer. Ecthyma, being more severe, may require several weeks to heal completely.
4) Does impetigo heal naturally?
In some cases, impetigo may resolve on its own without treatment. However, it is generally recommended to seek medical attention and receive appropriate treatment to speed up the healing process, reduce the risk of complications, and prevent the spread of the infection.
5) What ointment is good for impetigo?
The choice of ointment for impetigo depends on the severity and type of infection. Commonly prescribed topical antibiotics include mupirocin, retapamulin, or fusidic acid. These medications help eliminate the bacteria causing impetigo and promote healing of the affected skin.