What is Dermatomyositis?
‘Dermatomyositis-meaning’ is defined as a rare inflammatory disease that affects a person’s skin and muscles. It is classified as an autoimmune disorder, which means that the body’s immune system mistakenly attacks healthy tissues. Dermatomyositis primarily affects the skin, causing characteristic skin rashes, but it also affects the muscles, leading to muscle weakness and inflammation.
The exact cause of dermatomyositis rash is unknown, but it is believed to involve a combination of genetic and environmental factors. It can affect individuals of all ages, although it is more commonly diagnosed in adults and children between the ages of 5 and 15 or those in their 40s to 60s.
Dermatomyositis Symptoms
Understanding the symptoms associated with dermatomyositis is crucial for timely diagnosis and management. Here are some commonly observed dermatomyositis symptoms:
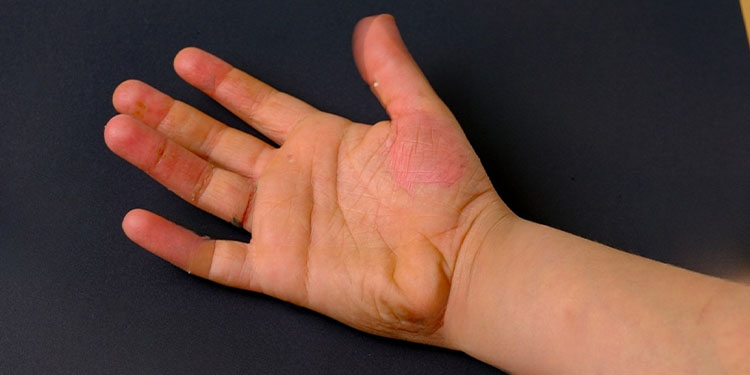
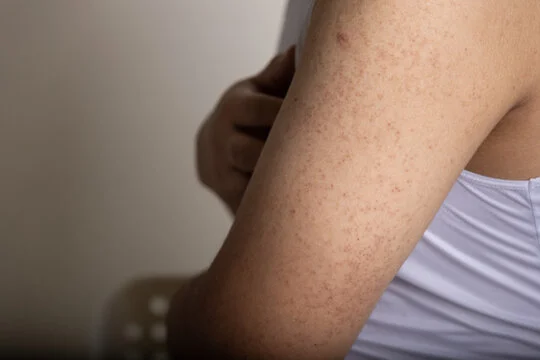
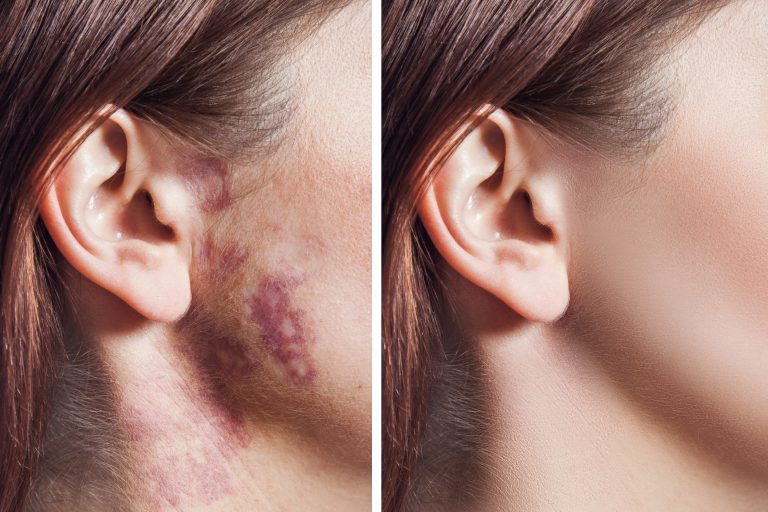
- Skin Changes: One of the hallmark symptoms of dermatomyositis is distinctive skin changes. These may include a rash that appears on the face, particularly on the eyelids and cheeks, as well as on the knuckles, elbows, knees, chest, and back. The rash often has a reddish or purplish colour and is known as “heliotrope rash.” Additionally, a scaly or raised rash can develop on the fingers, elbows, and knees, referred to as “Gottron’s papules”.
- Muscle Weakness: Dermatomyositis affects the muscles, leading to progressive muscle weakness. This weakness can affect both the proximal muscles and the distal muscles. Common signs of muscle weakness include difficulty in climbing stairs, getting up from a seated position, lifting objects, or raising the arms overhead.
- Muscle Pain and Inflammation: In addition to muscle weakness, individuals with dermatomyositis may experience muscle pain and skin inflammation. The affected muscles may feel tender and swollen. This pain and inflammation can contribute to reduced mobility and discomfort.
- Joint Pain and Swelling: Joint pain and swelling can occur in some cases of dermatomyositis. The joints most commonly affected are the wrists, fingers, and knees. The joint symptoms may resemble those of rheumatoid arthritis.
- Dysphagia: Difficulty in swallowing, known as dysphagia, can occur in dermatomyositis. It can make eating and drinking challenging and increase the risk of choking or aspiration.
- Fatigue: Many people with dermatomyositis experience persistent fatigue, which can significantly impact daily activities and quality of life. Fatigue is often unrelated to physical exertion and may not improve with rest.
- Shortness of Breath: In some cases, dermatomyositis can affect the muscles involved in breathing, leading to shortness of breath, especially during physical exertion.
Dermatomyositis Causes
The exact cause of dermatomyositis is currently unknown. However, it is believed to be an autoimmune disorder, which means that the body’s immune system mistakenly attacks its own healthy tissues. While the primary target of this immune response is the skin and muscles, dermatomyositis has also been associated with an increased risk of certain skin diseases and, in rare cases, skin cancer.
Here is an overview of the potential causes and factors associated with dermatomyositis:
- Genetic Factors: Although the role of genetics in dermatomyositis is not fully understood, there appears to be a genetic component involved. Certain genes may make individuals more susceptible to developing autoimmune disorders like dermatomyositis. However, further research is needed to identify the specific genes involved and their exact mechanisms.
- Environmental Triggers: Environmental factors may play a role in triggering dermatomyositis in individuals who are genetically predisposed. Potential triggers include viral or bacterial infections, such as a respiratory infection or exposure to certain medications or chemicals. However, the precise environmental triggers and their mechanisms in the development of dermatomyositis require more investigation.
- Autoimmune Response: In dermatomyositis, the immune system mistakenly identifies normal muscle and skin tissues as foreign and launches an immune response against them. This immune response leads to inflammation, muscle damage, and skin changes as a characteristic of the condition.
Dermatomyositis Diagnosis
Given the complex nature of dermatomyositis, an accurate diagnosis often requires a collaborative approach involving specialists from various fields, including dermatology, rheumatology, and other relevant disciplines coming together to check:
- Medical History: The healthcare professional will begin by discussing the individual’s symptoms, including any skin changes, muscle weakness, or other related complaints. They will inquire about the duration, progression, and severity of symptoms. It is important to provide a detailed medical history, including any past medical conditions, medications, family history of autoimmune diseases, and recent infections or exposures.
- Physical Examination: A thorough physical examination is conducted to assess the characteristic skin changes associated with dermatomyositis, such as the heliotrope rash, Gottron’s papules, and other skin findings. The healthcare professional will also evaluate muscle strength, range of motion, and signs of muscle inflammation or weakness.
- Blood Tests: Blood tests are commonly performed to assess specific markers that may indicate dermatomyositis. These may include:
- Creatine kinase (CK) levels: Elevated CK levels indicate muscle damage or inflammation.
- Antinuclear antibodies (ANA): These antibodies are frequently present in individuals with autoimmune disorders.
- Autoantibodies: Specific autoantibodies, such as anti-Jo-1, anti-Mi-2, or anti-MDA5, may be detected in dermatomyositis and can help with diagnosis and classification.
- Electromyography (EMG): EMG is a test that evaluates the electrical activity of muscles. It can help determine if there is muscle weakness, damage, or inflammation. EMG findings, along with the clinical presentation, can aid in the diagnosis of dermatomyositis.
- Muscle Biopsy: A muscle biopsy may be recommended to assess muscle tissue for signs of inflammation, degeneration, or other characteristic changes seen in dermatomyositis. The biopsy involves removing a small sample of muscle tissue for laboratory analysis.
- Imaging Studies: In some cases, imaging studies such as magnetic resonance imaging (MRI) or ultrasound may be performed to assess muscle involvement and detect areas of inflammation or damage.
Dermatomyositis Treatment
Similar to the diagnosis, dermatomyositis treatment also involves a multidisciplinary approach and may vary depending on the severity of symptoms, the extent of organ involvement, and individual factors.
Here are some common treatment options for dermatomyositis:
Medications:
-
- Corticosteroids: High-dose oral or intravenous corticosteroids are often the first line of treatment to suppress inflammation and control symptoms.
- Immunosuppressants: Medications such as methotrexate, azathioprine, mycophenolate, or rituximab may be prescribed to reduce immune system activity and control inflammation.
- Biologic agents: In certain cases, biologic agents like intravenous immunoglobulin (IVIG) or tumour necrosis factor (TNF) inhibitors may be considered for their immunomodulatory effects.
- Topical treatments: Medications such as topical corticosteroids or calcineurin inhibitors can be used to manage skin symptoms.
- Physical Therapy: A tailored exercise program supervised by a physical therapist can help improve muscle strength, flexibility, and overall physical functioning. It may include specific exercises, stretching, and range-of-motion activities.
- Occupational Therapy: Occupational therapy can assist individuals in maintaining independence in daily activities and provide strategies to manage any physical limitations.
- Sun Protection: Protecting the skin from sun exposure is crucial, as individuals with dermatomyositis may be more sensitive to sunlight. Wearing protective clothing, using sunscreen, and following a skincare routine can help minimise skin symptoms.
- Supportive Measures: In addition to medical interventions, supportive measures play a significant role in managing dermatomyositis. These may include adequate rest, managing stress, maintaining a balanced diet, and addressing associated comorbidities such as lung or heart involvement.
Conclusion
Dealing with dermatomyositis can be challenging, but you don’t have to face it alone. It’s important to connect with a dermatologist or rheumatologist who specialises in autoimmune diseases and can provide the expertise and support you need.
If you suspect you may have dermatomyositis or have already been diagnosed, finding a local dermatologist who understands your condition is crucial. Luckily, you can easily locate a skilled dermatologist in your area by visiting the Find Local Dermatologist webpage on our website.
Remember, early diagnosis and proper treatment are vital in managing dermatomyositis. So, don’t hesitate to find a local dermatologist who can be your trusted partner in this process. Take the first step today and find the right dermatologist for you. You’re not alone in this—better health and well-being are within reach!
FAQs on Dermatomyositis
1) What happens to your body when you have dermatomyositis?
Dermatomyositis is an autoimmune disease that primarily affects the muscles and skin. It can cause muscle weakness, inflammation, and characteristic red rashes on the skin. In some cases, it may also affect other organs such as the lungs, heart, or gastrointestinal tract.
2) Is dermatomyositis serious?
Yes, dermatomyositis can be a serious condition. It requires proper medical management as it can impact muscle function and quality of life.
3) Can you live a normal life with dermatomyositis?
While living with dermatomyositis may present challenges, many individuals can lead fulfilling lives with proper medical care. Treatment aims to control symptoms, manage inflammation, and preserve muscle function. With appropriate management and lifestyle adjustments, it is possible to maintain a good quality of life.
4) How do you diagnose dermatomyositis?
Diagnosing dermatomyositis involves a combination of factors, including a thorough physical examination, assessment of characteristic skin changes, evaluation of muscle strength and function, blood tests to check for specific antibodies and muscle enzymes, and sometimes additional imaging studies or muscle biopsies.
5) Can dermatomyositis be prevented?
At present, there is no known way to prevent dermatomyositis. It is an autoimmune disease, and the exact cause is not fully understood. However, certain lifestyle choices such as protecting the skin from excessive sun exposure and maintaining overall good health may help minimise the risk of developing complications associated with dermatomyositis.