Authors:
A Bansal, V Mahajan, N Sharma, N Sud, A Lath, N Gupta
Citation:
A Bansal, V Mahajan, N Sharma, N Sud, A Lath, N Gupta. Epidermolysis bullosa pruriginosa: Report Of A Rare Case. The Internet Journal of Dermatology. 2007 Volume 6 Number 2.
Introduction
A common but not clearly understood skin problem involving hypertrophic lesions and a lot of itching is referred to as Epidermolysis bullosa prurugenosa (EBP). People suffering from this skin condition experience physical as well as mental distress.
Here we are going to talk about the case of a 40 year old man affected by EBP and the treatment course.
What is EBP?
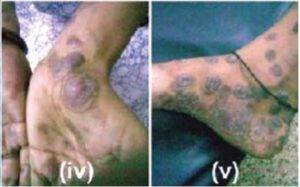
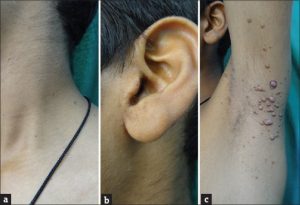
Before looking for an effective treatment of EBP, it is important to know more about this problem. Its full name is Epidermolysis bullosa pruriginosa. The major symptoms of this skin condition are blisters, skin fragility, scars , nail dystrophy and nodular lesions. Usually these symptoms are visible and concentrated on the forearms and shins. Widespread lesions can be seen along with severe pruritus or skin itching.
Onset
The problem may commence as early as childhood and start becoming more pronounced as the person becomes older, especially when he or she reaches the 20s or the 30s. This case study is about a 40 year old man who suffers from the problem of EBP. He was treated successfully with betamethasone valerate and fucidic acid based ointment and oral cetrizine.
Case report
The patient, a 40 year old male is a child of non-consanguineous parents, that is, the parents are not related to each other. The pregnancy was normal and the delivery was uneventful. Since childhood, the person had symmetrical, severe skin itching and overgrowing and enlarging lesions on extremities. The problem of of severe itching of the skin became a major cause of embarrassment and the person was unable to enjoy sound sleep. As per his case history, he had small blisters developing on his extremities after a minor trauma he suffered in his childhood. These blisters would rupture and would subsequently heal, leaving a lot of scars behind giving an ugly appearance. Although the blisters susbsequently reduced in frequency and intensity as he aged, but he started developing severely itchy nodular plaques. If his case history is taken into consideration, this problem could not have been due to drug or food allergy, atropy or cell degeneration, a systemic or cutaneous disorder. No problem was faced by his siblings and parents. Initially, he was put on antihistamines and systemic or topical steroids, but it gave relief temporarily.
Case presentation
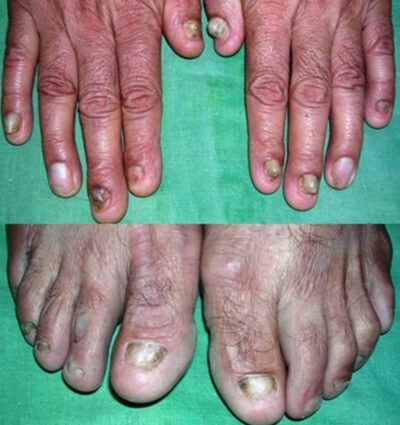
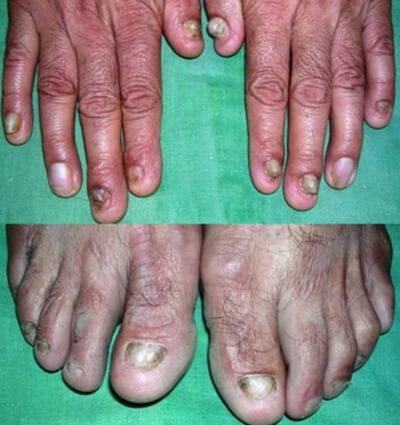
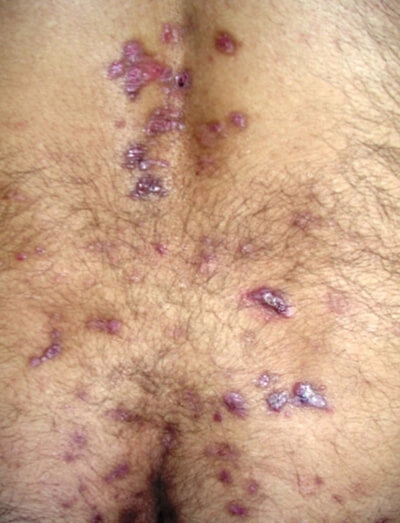
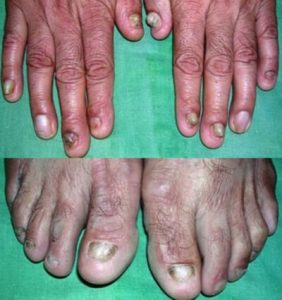
When the patient’s skin was thoroughly examined, several hardened, damaged and thickened pimples were noticed that formed plaques in straight lines over the extensor surfaces that is the skin on the joint’s opposite side of the lower back and shins. The forearms also showed some isolated lesions, but no scars and lesions were seen on the face and there was no problem in bending and curving. In between these lesions, scarring, freshly scratched and eroded lesions and abrasions of the skin was seen. The nails of the fingers and toes were partially lost. No abnormality was seen in mucosae and hair.
Clinical diagnosis
After conducting a battery of routine tests that included serum biochemistry, complete blood count, chest x rays and urinalysis, everything was found normal. Mild abnormalities were seen in the biopsy specimen taken from a lesion in the shin area through histopathologic examination. Only a mild inflammation was noticed in the middle and upper dermis.
Course of treatment
On the basis of histologic and clinical features, EBP was diagnosed in the patient and he was counselled for anylatical and genetic implications that may be possible when suffering from this problem. Oral cetrizine 10 mg b.i.d and application of betamethasone valerate 1 percent and fucidic acid 2 percent was prescribed twice in a day.
Results
Significant improvement was seen in the patient after 6 months of regular medication and the frequency of new blisters decreased.
Discussion
Many people suffer from skin problems but don’t take it seriously and think that these will go away, but, in reality, a delay in getting the problem diagnosed and treated results in the problem becoming more severe and pronounced. As in the case of this patient suffering from EBP, who suffered great agony.
Cases such as this one are very infrequent in nature. Also, the age when a person may suffer from this problem varies greatly. It the problem occurs right after birth, it may manifest in not so severe blisters on the extremities. Sometimes, a person may also show the symptoms of this condition in adulthood.
Since there are many factors like environmental, genetic, hormonal, immunological and systemic and cutaneous factors that may be responsible for the onset of EBP problem, its clinical course is difficult to predict. It is very rare to find frank blisters. This patient had all pathological and clinical features and it seems that the disorder was inherited sporadically. The reason behind severe itching was attributed to iron deficiency, atropy, thyroid dysfunction or abnormal reactivity on the dermis. At the same time there was no widespread abnormality seen connected with EBP cases. Severe itching is the major feature of this condition.
It is very difficult to manage EBP clinically because of the absence of specific therapies. The problem with this condition is that new lesions will still continue to appear even in the face of aggressive treatment. Though new approaches to treat this condition are coming up, it is recommended that any skin condition must be immediately diagnosed and treated, lest it escalate further to become a severe medical condition.
Disclaimer: This case study is meant for understanding purpose. Consumers are advised not to do self medication and meet their dermatologists for any type of skin problem.